Hi fellow CMIOs, CNIOs, and other #HealthIT and Applied Clinical #Informatics friends,
Today’s post is short, but one that I think most clinical friends will understand and appreciate. For conceptual teaching purposes only, I’m going to ask the question:
Here’s my theory: Clinicians may actually have an advantage here. If you’ve ever studied the human heart — its anatomy, its functions, its biology, and its electrophysiology — you already know a lot about teamwork, workflow design, clinical operations, and essentially how to get things done.
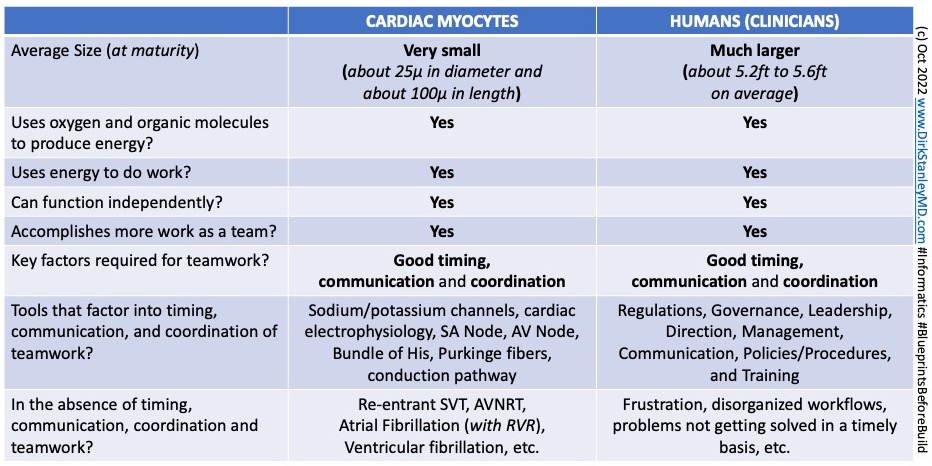
After all, cardiac myocytes and humans (clinical leaders and team members) work towards a common goal. We both can function as individual units, but we function even better together as a well-organized, well-synchronized team:
Let’s face it, healthcare is a team sport. So when I’m working with other clinical leaders — especially new ones — for support, I often remind them of the importance of the infrastructure and tools that we sometimes take for granted.
- Regulations (both Federal and State)
- Governance (e.g., Committee structures)
- Leadership
- Direction
- Management
- Communication
- Bylaws
- Policies/Procedures
- Training/Onboarding
- Continuing Education
- Offboarding
- Teamwork
After all, when growing a plant, it’s not just the seeds you need to worry about, it’s also the soil. Without enough of this ‘supporting soil’ (the tools above) in place, it becomes very easy to run into problems growing the seeds. And so, for end-users, managers, directors, leaders, and executives alike, this can sometimes result in loss of efficiency, frustration, disorganized workflows, problems not getting solved on a timely basis, etc.
Typically, these tools don’t get enough attention from new clinical leaders. The reason is that until they’re in a leadership position, their focus is largely on ‘clinical things’ like working with patients, diagnosing and treating diseases, performing operations and procedures, etc. While those are all the reasons we are in healthcare, it’s still important to understand the many ‘non-clinical’ tools that make those things happen. (In truth, those tools are just as clinical as penicillin. But due to time constraints, they usually don’t teach much about them in medical schools.)
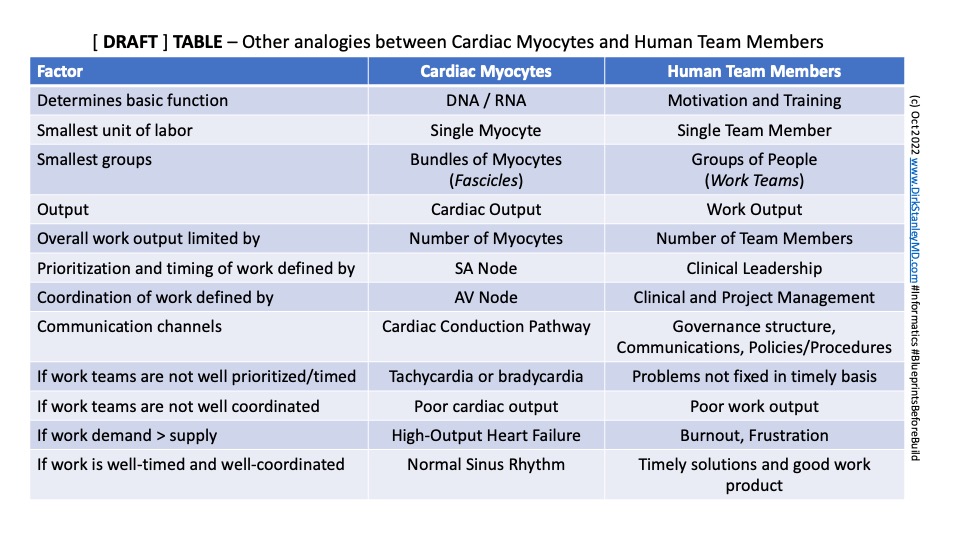
What I find especially interesting is that, as a physician who during my career has treated cardiac tachyarrhythmias at the bedside (using beta-blockers, calcium-channel blockers, adenosine, cardioversion, etc.), there are similar analogous ways to treat these same ‘human tachyarrhythmia’ problems on project teams.
And so, when I have the opportunity to teach a new clinical leader about how to solve problems and function in teams, I simply remind them that modern human biology has evolved over thousands of years to solve these same sorts of problems that we experience in healthcare today. Therefore, sometimes looking inward with a microscope is just as helpful as looking outward with a telescope.
Finally, my good friend, and one of my clinical informatics colleagues, Stefanie Shimko-Lin, BSN, RN, once shared this cardiac analogy with me: “Collateral circulation is a workaround, that happens when the desired workflow doesn’t work. If you make it easy to do the right thing, people will do it.”
These analogies may all seem a bit peculiar and tongue-and-cheek. But if you’re a clinical leader, I hope this blog post helps to spark helpful discussion and learning with your own clinical leadership and project teams, so that you can better solve the workflow and operational issues you might encounter in your daily clinical routines.
This piece was written Dirk Stanley, MD, a board-certified hospitalist, informaticist, workflow designer, and CMIO, on his blog, CMIO Perspective.



Share Your Thoughts
You must be logged in to post a comment.